 |
 |
| Korean J Ophthalmol > Volume 36(6); 2022 > Article |
|
Abstract
Purpose
To evaluate the dynamic range of retinal nerve fiber layer (RNFL) and optic nerve head (ONH) parameters measured using optical coherence tomography (OCT) in conditions ranging from nonglaucomatous status to advanced glaucoma by longitudinal observation.
Methods
A total of 15 eyes from 12 participants with glaucoma progression from a nonglaucomatous status to advanced glaucoma were included. The RNFL and ONH parameters were compared between the nonglaucomatous and advanced stages within the same eye. The absolute and relative changes in OCT parameters were analyzed.
Results
The median highest intraocular pressure was 42.5 mmHg (interquartile range, 37.5 to 54.5 mmHg), and the final mean deviation of the visual field test was −24.68 dB (interquartile range, −23.93 to −31.13 dB). The median relative changes in RNFL thickness were −40.6% in the overall area, and −51.9%, −21.4%, −51.1%, and −41.8% in the superior, nasal, inferior, and temporal quadrants, respectively (all p < 0.05). Relative changes in the rim area, disc area, average cup to disc ratio, vertical cup to disc ratio, and cup volume were −56.64%, 0.59%, 62.10%, 66.0%, and 337.90%, respectively (all p < 0.05, except for disc area with a p-value of 0.753).
Conclusions
The dynamic range of the RNFL thickness ranged from 40.6% to 51.9%, and the dynamic range of the ONH parameters ranged from 56.64% to 337.90%. During the course of glaucoma progression, the cup volume showed the widest dynamic range. However, the disc area did not show significant changes.
Glaucoma is characterized by progressive changes in the optic nerve head (ONH), retinal nerve fiber layer (RNFL), retinal ganglion cells (RGCs), and the corresponding visual field. Optical coherence tomography (OCT) is a widely used technique for the measurement of ONH parameters, circumpapillary RNFL thickness, and macular RGC thickness. To identify the severity of structural damage, it is important to investigate the dynamic range of ONH parameters, RNFL thickness, and RGC thickness measured by OCT. Previous cross-sectional studies evaluated the dynamic range of OCT parameters by comparing healthy eyes and eyes with glaucoma at various stages [1-5]. However, comparison of clinical data in different patients may be affected by various ocular and systemic factors. Thus, the ideal way to assess the dynamic range of OCT parameters according to glaucoma development and progression may be to observe longitudinal changes in OCT parameters within the same eye from nonglaucomatous status to advanced glaucoma. This study was performed to assess the dynamic range of ONH parameters and RNFL thickness in the same eye in a longitudinal manner using OCT.
This retrospective observational study was approved by the Institutional Review Board of Chungnam National Univeristy Hospital (No. 2022-01-028-003). All the procedures conformed to the guidelines of the Declaration of Helsinki. The requirement for informed consent was waived because of the retrospective study design.
Participants with glaucoma progressing from a nonglaucomatous to an advanced stage within the same eye were included in the study. Detailed ophthalmic examinations, including measurements of the refractive error, visual acuity, and intraocular pressure (IOP) using a Goldmann applanation tonometer, slit-lamp biomicroscopic examination, fundus photography, and automated visual field test using a Humphrey Field Analyzer (Carl Zeiss Meditec, Dublin, CA, USA) with the Swedish interactive thresholding algorithm, were performed. Fixation losses and false-positive and false-negative response rates of less than 20% were considered to indicate reliable visual fields. OCT examination was performed using Cirrus high-definition spectral domain OCT (Cirrus HD-OCT, Carl Zeiss Meditec) to measure circumpapillary RNFL thickness, ONH parameters, and macular RGC thickness.
The inclusion criteria were as follows: (1) age ≥ 18 years, (2) ONH without glaucomatous changes (i.e., a cup to disc ratio of >0.7 and neuroretinal rim narrowing) in fundus photographs and no RNFL defect on fundus photographs at the initial visit (nonglaucomatous status), and (3) advanced glaucoma at the final visit. Advanced glaucoma was defined as a mean deviation (MD) of visual field test results worse than −12 dB [6]. The type of glaucoma was not restricted; all types of glaucoma, including primary open-angle glaucoma, angle-closure glaucoma, neovascular glaucoma, and uveitic glaucoma were enrolled. Any treatment for IOP control, including medication, laser therapy, or surgery, was performed according to each eye’s condition. Eyes with coexisting retinal disorders (i.e., diabetic retinopathy, macular degeneration, or retinal vascular disorders) were not excluded if they did not affect ONH or RNFL thickness measurements. The presence of optic neuropathies other than glaucoma (i.e., compressive, traumatic, ischemic, or congenital optic neuropathies) was considered an exclusion criterion.
A 200 × 200 cube optic disc scan and macula scan were obtained using Cirrus HD-OCT [7]. To acquire the images, the scanning laser was focused after the participants were seated and properly positioned within the chin rest. Using the iris and fundus views, the ONH or macula was aligned so that it was presented at the center of the scan. Once the ONH or macula was centered on the live scanning laser image, data from a 6 × 6-mm area were captured. The Cirrus HD-OCT algorithm automatically determines the vitreoretinal surface and posterior boundary of the RNFL and presents circumpapillary RNFL thickness values of the overall area (average) and four quadrants (superior, nasal, inferior, and temporal). Various ONH parameters, including the rim area, disc area, average cup to disc ratio, vertical cup to disc ratio, and cup volume, were automatically generated by the Cirrus HD-OCT algorithm. Cirrus HD-OCT automatically segments the anterior border of the inner plexiform layer and posterior border of the RGC and shows average, minimum, and sector-based (superotemporal, superior, superonasal, inferonasal, inferior, and inferotemporal) macular ganglion cell-inner plexiform layer (GCIPL) thickness values. Images with segmentation errors, artifacts with vitreous opacity, or signal strengths <7 were excluded.
The number of included eyes (15 eyes) was insufficient for parametric analyses. Therefore, the variables are presented as median and interquartile range. The absolute change was defined as the parameter at the final visit minus the parameter at the initial visit, and the relative change (%) was defined as the following: [(parameter at the final visit) − (parameter at initial visit)]/(parameter at initial visit) × 100. Differences between the baseline test and the final test were analyzed using the Wilcoxon signed-rank test. The threshold for statistical significance was set at p < 0.05. Statistical analyses were performed using IBM SPSS ver. 26.0, (IBM Corp., Armonk, NY, USA).
A total of 15 eyes from 12 participants (two female and 10 male participants) were enrolled. The median age was 53.5 years (interquartile range, 39.3 to 70.5 years), and all participants were Korean. Among the images of the 15 eyes, macular GCIPL thickness analysis was available for only five eyes; the other eyes had segmentation errors in GCIPL thickness determination. Therefore, in the present study, only ONH parameters and RNLF thickness were analyzed. The distribution of glaucoma types was primary open-angle glaucoma in two eyes, neovascular glaucoma in three eyes, uveitic glaucoma in five eyes, steroid-induced glaucoma in two eyes, angle-closure glaucoma in two eyes, and secondary glaucoma after ocular trauma in one eye. To control IOP, trabeculectomy, Ahmed glaucoma valve (New World Medical, CA, USA) implantation, selective laser trabeculoplasty, or cyclophotocoagulation was performed in 14 eyes. The median follow-up period was 52.0 months (interquartile range, 43.0 to 95.0 months). The median baseline IOP was 40.0 mmHg (interquartile range, 27.0 to 52.0 mmHg), the median highest IOP was 42.5 mmHg (interquartile range, 37.5 to 54.5 mmHg), and the final MD of the visual field test was −24.68 dB (interquartile range, −23.93 to −31.13 dB) (Table 1).
All RNFL thickness parameters showed significant differences between the baseline and final visits (p < 0.001) (Fig. 1A-1E and Table 2). The median average RNFL thickness at the baseline visit was 100.0 μm (interquartile range, 95.0 to 111.0 μm) and decreased to 62.0 μm (interquartile range, 55.0 to 64.0 μm) at the final visit. The median absolute (relative) changes in the average, superior, nasal, inferior, and temporal quadrant RNFL thickness were −36.0 (−40.6%), −67.0 (−51.9%), −18.0 (−21.4%), −61.0 (−51.1%), and −37.0 μm (−41.8%), respectively (Table 2).
Among the ONH parameters, the rim area, disc area, average cup to disc ratio, vertical cup to disc ratio, and cup volume significantly changed (p < 0.01); however, the disc area did not show a significant change (p = 0.753) (Fig. 2A-2E and Table 2). The median relative changes in the rim area, disc area, average cup to disc ratio, vertical cup to disc ratio, and cup volume were −56.64%, 0.59%, 62.10%, 66.0%, and 337.90%, respectively (Table 2).
In the present study, the dynamic range of RNFL thickness ranged from 40.6% to 51.9%, and the dynamic range of the ONH parameters ranged from 56.64% to 337.90%. During the course of glaucoma progression, the cup volume showed the widest dynamic range. However, the disc area did not show significant changes. To the best of our knowledge, this is the only study to report longitudinal changes in RNFL and ONH parameters measured by OCT from nonglaucomatous status to advanced glaucoma.
To investigate the dynamic range of RNFL thickness, RNFL thickness of healthy eyes and glaucomatous eyes at various stages were analyzed [1-5]. For instance, a recent study using Cirrus HD-OCT reported that the average RNFL thickness reached a floor of 60.1 μm thickness at a visual field MD of −17.8 dB and the absolute and relative dynamic range was 28.1 μm and 31.8%, respectively [4]. The RNFL thickness in conditions with advanced glaucoma (measurement floor) may be explained by residual capillaries, astrocytes, and Müller cells after axonal loss [8,9]. Another study using Cirrus HD-OCT reported that the floor of the average, superior, and inferior RNFL thickness was 57.0, 65.0, and 61.2 μm, relatively, with an absolute dynamic range of 35.4, 54.5, and 56.7 μm, respectively, at a visual field MD of −22.2 dB [3]. In the present study, the average, superior, nasal, inferior, and temporal quadrant RNFL thickness with advanced glaucoma was 62.0, 67.0, 63.0, 65.0, and 48.0 μm, respectively, at a visual field MD of −24.68 dB. The dynamic range presented as an absolute (relative) change in the average, superior, nasal, inferior, and temporal quadrant RNFL thickness was −36.0 (−40.6%), −67.0 (−51.9%), −18.0 (−21.4%), −61.0 (−51.1%), −37.0 μm (−41.8%), respectively. These ranges were similar to those of a previous study with a cross-sectional design [3,4].
The relative dynamic ranges of the nasal (−21.4%) and the temporal quadrant RNFL (−41.8%) were lower than those of the superior (−51.9%) and the inferior quadrants (−51.1%). This finding may be explained by the preferential occurrence of RNFL loss in the superior and inferior quadrants. Therefore, RNFL thickness changes in the nasal and temporal quadrants may have a lower ability to detect progression than the superior or inferior RNFL thickness.
Previous studies evaluating the dynamic range of OCT parameters have focused on the circumpapillary RNFL or macular RGC thickness [1-5]. Little is known about the dynamic range of ONH parameters. In the present study, the median rim area, cup to disc ratio, and cup volume at final visit was 0.58 mm2, 0.82, and 0.579 mm3, respectively. Previous studies assessing ONH parameters in advanced glaucoma showed similar results [10,11]. For instance, in a study by Lavinsky et al. [10], the mean rim area, cup to disc ratio, and cup volume of eyes with advanced glaucoma was 0.65 mm2, 0.78, and 0.50 mm3, respectively. When longitudinal change was evaluated, the median relative dynamic range of the rim area, cup to disc ratio, and cup volume was −56.64%, 64.10%, and 337.90%, respectively. These ranges were greater than those of the RNFL thickness. In particular, cup volume showed the widest dynamic range. The RNFL mainly consists of axons of RGCs. In contrast, large retinal vessels, including the trunk and prelaminar tissue, are present in the optic cup, in addition to the neuroretinal rim. Thus, in addition to axonal changes in RGCs (RNFL, rim), changes in vascular and connective tissues may coexist in the optic cup. This may contribute to a wider dynamic range of cup volumes than the other parameters.
In contrast to the other ONH parameters, the disc area did not show a significant change during the course of glaucoma development and progression. Belghith et al. [12] investigated longitudinal changes in the location of Bruch’s membrane opening (BMO), which corresponds to the disc area automatically determined by the Cirrus HD-OCT algorithm from healthy status to an early glaucoma stage, and also reported that the BMO location was stable. Sharma et al. [13] reported that the BMO area did not change with acute IOP elevation. Thus, BMO may be considered as an anatomic reference for the measurement of various ONH parameters, such as ONH surface depth, anterior lamina cribrosa surface depth, and prelaminar tissue thickness [14]. Our study results further suggest that disc area determined by BMO location may be less affected than other parameters, even in an advanced stage of glaucoma.
Macular RGCs have been reported to have a wider dynamic range than RNFL thickness, especially in advanced glaucoma [4,5]. Therefore, the assessment of the dynamic range of macular RGC thickness may provide useful information. Unfortunately, in the present study, RGC thickness analysis of sufficient quality was available in only five eyes. In the majority of cases, artifacts and segmentation errors related to various retinopathies or abnormal thickening caused by macular edema were found. Among the 15 eyes, three had diabetic retinopathy with a history of panretinal photocoagulation. This might have contributed to the visual field test results. However, all of these eyes exhibited visual field losses of less than 10°, which may be mainly explained by glaucoma. Therefore, eyes with diabetic retinopathy were not excluded.
In the present study, 14 of 15 eyes underwent glaucoma surgery or laser treatment. A sudden drastic IOP decrease due to glaucoma surgery may affect the OCT parameters, especially in the early postoperative period. Therefore, the results of the present study may show different OCT change patterns compared with the conditions without surgical intervention. The median follow-up period showed a wide range of 20 to 109 months. Moreover, the number and intervals between visits were variable and 14 of 15 eyes underwent surgical intervention during the follow-up period, which might have affected OCT parameters, especially in the early postoperative period. Unfortunately, the present study enrolled only 15 eyes, which would hinder adjusting various affecting factors (i.e., number of tests, interval of tests, intervals between the operation and OCT test, and intereye correlation). Therefore, only data from the initial and final visits were analyzed using nonparametric statistical analyses. Further studies investigating longitudinal changes in OCT parameters, including RGC thickness, with a greater number of patients from nonglaucomatous status to advanced glaucoma may be needed. Recent studies have reported that OCT angiography parameters showed different dynamic range patterns in the RNFL or RGC [4,5]. We hope that further studies examining the longitudinal changes in OCT angiography parameters will be performed.
In conclusion, the dynamic range of RNFL thickness from a nonglaucomatous status to advanced glaucoma by longitudinal observation showed results similar to those of previous cross-sectional studies. When the dynamic range of the ONH parameters was evaluated, cup volume showed the widest range, and disc area showed the smallest change. These findings may be helpful for the assessment of glaucoma in clinical practice.
References
1. Hood DC, Kardon RH. A framework for comparing structural and functional measures of glaucomatous damage. Prog Retin Eye Res 2007;26:688-710.



2. Mwanza JC, Budenz DL, Warren JL, et al. Retinal nerve fibre layer thickness floor and corresponding functional loss in glaucoma. Br J Ophthalmol 2015;99:732-7.



3. Mwanza JC, Kim HY, Budenz DL, et al. residual and dynamic range of retinal nerve fiber layer thickness in glaucoma: comparison of three OCT platforms. Invest Ophthalmol Vis Sci 2015;56:6344-51.



4. Phillips MJ, Dinh-Dang D, Bolo K, et al. Steps to measurement floor of an optical microangiography device in glaucoma. Am J Ophthalmol 2021;231:58-69.



5. Moghimi S, Bowd C, Zangwill LM, et al. Measurement floors and dynamic ranges of OCT and OCT angiography in glaucoma. Ophthalmology 2019;126:980-8.



6. Hodapp E, Parrish RK, Anderson DR. Clinical decisions in glaucoma. St. Louis: Mosby; 1993.
7. Song MY, Hwang YH. Interocular symmetry of optical coherence tomography parameters in healthy children and adolescents. Sci Rep 2022;12:653.




8. Varela HJ, Hernandez MR. Astrocyte responses in human optic nerve head with primary open-angle glaucoma. J Glaucoma 1997;6:303-13.


9. Wang L, Cioffi GA, Cull G, et al. Immunohistologic evidence for retinal glial cell changes in human glaucoma. Invest Ophthalmol Vis Sci 2002;43:1088-94.

10. Lavinsky F, Wu M, Schuman JS, et al. Can macula and optic nerve head parameters detect glaucoma progression in eyes with advanced circumpapillary retinal nerve fiber layer damage? Ophthalmology 2018;125:1907-12.



11. Hu H, Li P, Yu X, et al. Associations of ganglion cell-inner plexiform layer and optic nerve head parameters with visual field sensitivity in advanced glaucoma. Ophthalmic Res 2021;64:310-20.



12. Belghith A, Bowd C, Medeiros FA, et al. Does the location of bruch’s membrane opening change over time? Longitudinal analysis using san diego automated layer segmentation algorithm (SALSA). Invest Ophthalmol Vis Sci 2016;57:675-82.



Fig. 1
Changes in the (A) average, (B) superior, (C) nasal, (D) inferior, and (E) temporal quadrant retinal nerve fiber layer (RNFL) thickness from a nonglaucomatous status (baseline) to an advanced stage of glaucoma (final visit). Each line indicates the changes in the RNFL thickness in each eye.
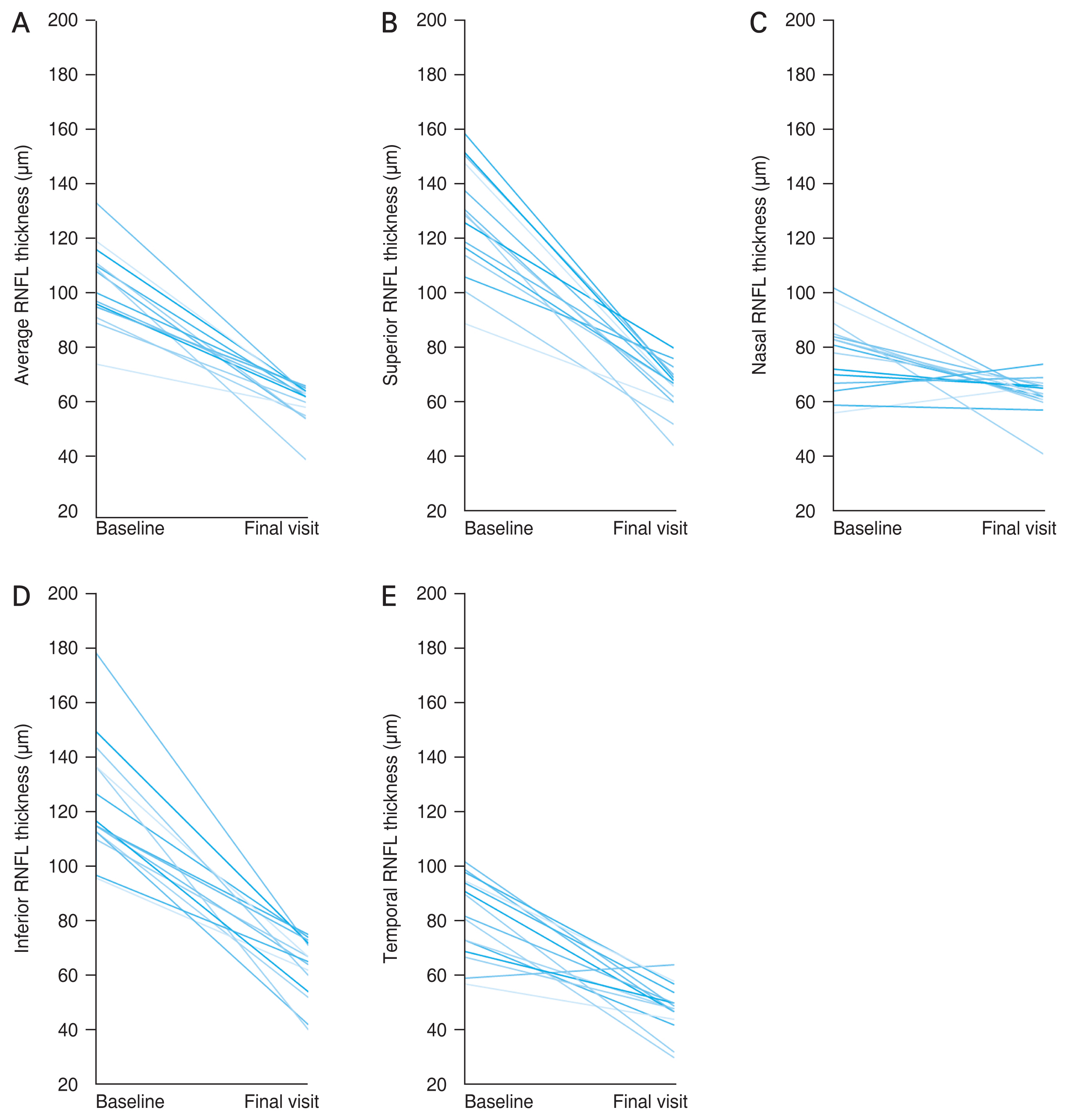
Fig. 2
Changes in the optic nerve head parameters from a nonglaucomatous status (baseline) to an advanced stage of glaucoma (final visit). Optic nerve head parameters are (A) the rim area, (B) the disc area, (C) the average cup to disc ratio, (D) the vertical cup to disc ratio, and (E) the cup volume. Each line indicates the changes in optic nerve head parameters in each eye.

Table 1
Clinical characteristics of eyes (n = 15)
Table 2
Changes in RNFL thickness and ONH parameters
| Variable | Baseline visit | Final visit | Dynamic range | Relative range (%) | p-value* |
|---|---|---|---|---|---|
| RNFL thickness (μm) | |||||
| Average | 100.0 (95.0 to 111.0) | 62.0 (55.0 to 64.0) | −36.0 (−56.0 to −29.0) | −40.6 (−50.0 to −32.6) | 0.001 |
| Superior | 129.0 (114.0 to 148.0) | 67.0 (60.0 to 70.0) | −67.0 (−82.0 to −46.0) | −51.9 (−55.3 to −38.7) | 0.001 |
| Nasal | 81.0 (67.0 to 85.0) | 63.0 (61.0 to 66.0) | −18.0 (−25.0 to −2.0) | −21.4 (−29.4 to −3.4) | 0.004 |
| Inferior | 115.0 (113.0 to 137.0) | 65.0 (54.0. 72.0) | −61.0 (−78.0 to −42.0) | −51.1 (−58.3 to −36.5) | 0.001 |
| Temporal | 82.0 (69.0 to 98.0) | 48.0 (44.0 to 54.0) | −37.0 (−52.0 to −19.0) | −41.8 (−52.5 to −28.4) | 0.002 |
| ONH parameter | |||||
| Rim area (mm2) | 1.13 (1.06 to 1.49) | 0.58 (0.41 to 0.74) | −0.64 (−0.97 to −0.33) | −56.64 (−65.00 to −30.28) | 0.001 |
| Disc area (mm2) | 1.99 (1.45 to 2.05) | 1.81 (1.66 to 2.07) | 0.01 (−0.06 to 0.05) | 0.59 (−2.63 to 2.50) | 0.753 |
| Average cup to disc ratio | 0.53 (0.40 to 0.69) | 0.82 (0.77 to 0.89) | 0.35 (0.11 to 0.42) | 62.10 (18.03 to 105.41) | 0.001 |
| Vertical cup to disc ratio | 0.54 (0.37 to 0.66) | 0.82 (0.79 to 0.86) | 0.35 (0.13 to 0.47) | 66.0 (18.6 to 127.03) | 0.001 |
| Cup volume (mm3) | 0.133 (0.065 to 0.299) | 0.579 (0.488 to 0.705) | 0.435 (0.354 to 0.527) | 337.90 (51.22 to 810.77) | 0.001 |



 PDF Links
PDF Links PubReader
PubReader ePub Link
ePub Link Full text via DOI
Full text via DOI Full text via PMC
Full text via PMC Download Citation
Download Citation Print
Print




