 |
 |
| Korean J Ophthalmol > Volume 35(4); 2021 > Article |
|
Abstract
Purpose
To compare functional and anatomic outcome of intravitreal ranibizumab (IVR) and intravitreal aflibercept (IVA) treatments in neovascular age-related macular degeneration by using the treat and extend (TE) protocol.
Methods
In this retrospective chart study, treatment naïve 74 eyes of 74 age-related macular degeneration patients treated with IVR and IVA (38 eyes in IVR and 36 eyes in IVA group) with TE protocol were included. Following three consecutive monthly intravitreal injections, TE protocol was applied to each group. Patients were followed up for at least 36 months. Mean change in best-corrected visual acuity (BCVA), central macula thickness (CMT) and injection numbers over 3 years were compared.
Results
Among 36 months period, the mean number of injections was 17 ± 4 for both groups (p > 0.05). In terms of CMT, there was no statistically significant difference between groups at 36 months compared to baseline. A decrease of 72.55 ± 39.37 μm in CMT was detected in IVR group, whereas the decrease was 70.58 ± 33.96 μm in IVA group (p > 0.05). There was a significant increase in BCVA at 36 months of measurements. In addition, BCVA demonstrated an increase of 4.1 ± 0.44 letters in IVR group and 4.36 ± 0.67 letters in IVA group after 36 months compared to the baseline (p > 0.05).
Age-related macular degeneration (nAMD) is one of the most common reasons of blindness in developed countries due to aging population [1]. Increased permeability of the blood vessels and new vessel formation in the macula could play a major role in nAMD. It is known that vascular endothelial growth factor (VEGF)-A is responsible for these actions. Therefore, recent treatments regarding the blockage of VEGF-A have facilitated a dramatic improvement in these patients [2-5].
Intravitreal ranibizumab (IVR) and intravitreal aflibercept (IVA) exhibit an inhibitory effect on all isoforms of VEGF-A, which were approved in June 2006 and in November 2011 by Food and Drug Administration respectively [6,7]. Previous randomized controlled studies have revealed that a monthly injection of IVR and bi-monthly injection of IVA, after a loading dose of 3 monthly injections, result in greatest visual acuity gain [8-12]. A similar improvement in visual acuity was obtained with optical coherence tomography (OCT) guided pro re nata (PRN) administration in the Prospective Optical Coherence Tomography Imaging of Patients with Intraocular Ranibizumab (PrONTO) study [13].
PRN therapy can facilitate a diminished number of injections; however, disease recurrence should strictly be followed by monthly assessment visits. Among all protocols, the extended treatment intervals of a treat and extend (TE) protocol could alleviate the burden of both patients and clinics by optimizing the number of hospital visits and the overall number of injections. In TE protocol, treatment is initiated with a series of monthly loading doses. The treatment interval is then gradually extended in which the intervals between treatments are extended as long as the macula remains dry [14-16].
This study was designed to compare the long-term functional and anatomical effects of IVR and IVA administration by using TE protocol in patients with nAMD.
This study was a retrospective, consecutive case series and was approved by the institutional review board of T. C. Demiroglu Bilim University. Written informed consent was obtained from each subject following a detailed explanation of the objectives and protocol of the study, which was conducted in accordance with the ethical principles stated in the Declaration of Helsinki. Clinical data were obtained from nAMD patients who were treated in our institution between March 2015 and January 2019.
Patients who met all the following criteria were included in the study; demonstrating best-corrected visual acuity (BCVA) that range between 20 / 40 and 20 / 200 relying on Early Treatment Diabetic Retinopathy Study (ETDRS) chart, presence of leakage due to choroid neovascularization (CNV) or macular edema in fundus fluorescein angiography, having subretinal fluid, having cystic maculopathy or central macular thickness (CMT) of at least 250 μm on OCT (Optovue, Fremont, CA, USA) and not being treated for macular degeneration. In our clinical setting we do not use any special criteria for deciding intravitreal injection type. We included all patients who completed their follow-up period. Exclusion criteria were; existence of any disease other than AMD that might reduce BCVA (e.g., retinal angiomatous proliferation, polypoidal choroidal vasculopathy confirmed with indocyanine green angiography, myopic CNV); existence of pigment epithelium detachment without exudative symptoms; a history of vitrectomy for the subject eye; having retinal photocoagulation treatment until 1 month prior to the onset of the study; missing at least one control visit; aphakia or posterior capsule rupture; a history of glaucoma, having chronic renal failure and presence of bleeding diathesis. For all of the patients, the diagnosis of nAMD was confirmed by indocyanine green angiography. In the venous intermediate frame and the late frame CNV edges were manually contoured and measured.
All intraocular injections were performed in the operating room. Following administration of local proparacaine hydrochloride 0.5%, eye leashes and conjunctiva were cleaned with 5% povidone iodine. After inserting the speculum to keep the eye open, the drugs were injected through the limbus upper temporal quadrant, at 3.5 mm distance for pseudo-phakic/aphakic eyes and 4 mm distance for phakic eyes from limbus. All patients were prescribed a quinolone group of antibiotics, four times a day for 7 days.
IVR 0.5 mg/0.05 mL (Lucentis; Novartis Pharma AG, Basel, Switzerland) and IVA 2 mg/0.05 mL (Eylea; Bayer Pharma, Berlin, Germany) were injected monthly for 3 consecutive months. During each visit; BCVA and intraocular pressure were evaluated. In addition, CMT measurement via OCT was performed which is followed by biomicroscopic evaluation of anterior segment and examination of fundus. In case of absence of any signs of CNV activity, follow-up and treatment sessions were extended by 2 week-intervals after the loading phase. However, if any signs of activation (persistant or recurrent cystic changes, 100 μm or more increment in CMT, newly developed CNV, new hemorrhage, being unable to read five or more letters on ETDRS after the latest BCVA evaluation) were detected, treatment intervals would subsequently be shortened by 2 weeks. Anti-VEGF treatment was administered at every visit, regardless of CNV activity. The maximum interval between treatments was 12 weeks. Patients’ CMT and BCVA measurements compared at baseline, 12th, 24th, and 36th months.
Statistical analysis was performed by using IBM SPSS Statistics ver. 22.0 (IBM Corp., Armonk, NY, USA). The mean ± standard deviation and median (interquartile range) were rendered when assessing the study findings. The Kolmogorov-Smirnov test was employed to analyze the distributional behaviors of the data. A chi-squared test was used to analyze the differences between the IVR and IVA injections, while a t test was used to analyze the independent samples. The differences between the baseline and 12-month measurements were analyzed by using the Wilcoxon signed-rank test. The results were considered within a confidence interval of 95% and a significance level of p < 0.05.
The mean ages of 38 patients in the IVR group and 36 patients in the IVA group were 72.95 ± 5.23 and 74.911 ± 5.03 years old, respectively (p > 0.05). The baseline CMTs in the IVR and IVA groups were 365.68 ± 68.34 versus 362.89 ± 59.06 μm, respectively (p > 0.05). There was no statistically significant difference between groups in terms of BCVA measurements (IVR 53.8 ± 8.30 vs. IVA 54.28 ± 8.13 letters) and CNV size (IVR 1.8 ± 1.30 vs. IVA 1.7 ± 1.2 mm2). The rest of demographic data is shown in Table 1.
In terms of mean numbers of injections, no statistical difference found between groups (p > 0.05). Mean number of injections was 17.16 ± 3.98 in IVR group and 17 ± 4.13 in IVA group in 36 months (Fig. 1). In IVR group, 10%, 55%, and 60% patients received <5 intravitreal injections in the first, second and third year respectively. Also, In IVA group, 3%, 61%, and 63% patients received <5 intravitreal injections in the first, second and third year respectively (Fig. 2A, 2B).
The 36-month CMT measurement in the IVR group revealed a decrease of 72.55 ± 66.67 μm when compared to the baseline measurements, whereas a decrease of 70.58 ± 50.32 μm was determined in the IVA group; which were statistically significant for both groups (p < 0.05). However, there was no significant difference between the groups in terms of the baseline, 12, 24, and 36 months CMT measurements (p > 0.05) (Table 2 and Fig. 3, 4).
After 36 months, BCVA demonstrated an increase of 4.11 ± 5.92 letters in IVR group and 4.46 ± 6.77 letters in IVA group compared to the baseline (p = 0.000, p < 0.001). However, there was no significant difference between the groups in terms of the baseline, 12, 24, and 36 months BCVA measurements (p > 0.05) (Table 2 and Fig. 3, 4).
Three patients (7.8%) in IVR group and four patients in IVA group (11.1%) experienced sub-conjunctival hemorrhage. Transient IOP elevation after 15 minutes from application was detected in four patients (10.5%) in IVR group and four patients (11.1%) in IVA group which resolved without medication.
IVR is approved by Food and Drug Administration in June of 2006. Many studies concerning the determination of the frequency of injections which is required to protect vision have been reported in the literature [17,18]. MARINA and ANCHOR studies suggests monthly injections for patients with nAMD, however this protocol may cause an increased financial burden both for the patients but and the health system [8,19].
PrONTO study is probably the first study that establish a patient specific protocol. They used ranibizumab injections and they designed the study to decrease the number of visits. Even though they achieved better BCVA in 24 months, PRN regimen can place a high burden on patients/healthcare services due to the monthly monitoring visits. They performed an average of 9.9 injections in 24 months [13]. We also try to decrease the number of injections using TE protocol however it ended up giving an average of 17 injections in 36 months. After performing first three injections, we provided at least one injection in every 2 to 3 months.
The VEGF Trap-Eye: regarding the letter gains in the scope of BCVA improvement and CMT decrease, Investigation of Efficacy and Safety in Wet AMD 1 and 2 studies (VIEW 1 and 2) compared monthly injections of 0.5 mg of IVR, monthly injections of 2 mg of IVA, and bimonthly injections of IVA, after the initial 3-monthly injections of loading dose and determined no statistically significant difference between three groups after 1 year. The VIEW 1 study found letter gains in the scope of BCVA improvement of 8.1, 10.4, and 7.9 letters for the monthly IVR group, monthly IVA group, and bimonthly IVA group, respectively. The VIEW 2 study calculated the same parameter as 9.4, 7.6, and 8.9 letters, respectively. However, the decreases in the CMT were 117, 117, and 129 μm in the VIEW 1 study and were 139, 157, and 149 μm in the VIEW 2 study, respectively [10].
A study by Berg et al. [20] investigated long-term visual results of treatment with anti-VEGF agents (IVR, IVA, and intravitreal bevacizumab) for nAMD following a TE regimen. They concluded that treatment of nAMD patients with a TE modality provided improvement and stability of vision for several years. In their study, mean BCVA was significantly improved after 4 years of treatment for the entire group of patients (8.6 letters at year 3). But in this study, all patients were treated with bevacizumab during the 1st year and but were switched to ranibizumab treatment in the 2nd year. Also, aflibercept became available in the market from 6th year of study, after which only 16 eyes were switched from bevacizumab or ranibizumab to aflibercept treatment. After 8 years of follow-up, 74% of the patients were discontinued from the study. More than half of patients were discontinued from the study within the first 2 years of treatment [20]. In our study BCVA demonstrated an increase of approximately four letters after 36 months in both groups. The difference between the studies at year 3 can be explained with homogeneity of study groups, treatment naive patient selection and exclusion of switchers in our study.
Smit et al. [21] also compares both IVR and IVA in a TE protocol and did not show any difference between groups (0.012 vs. 0.17, p > 0.05 and 122% vs. 120%, p > 0.05), however they injected IVA every other month versus IVR every month and they observed the same BCVA improvement. In addition, Gillies at al. [22] performed a similar study like Garweg et al. [23] and Smit et al. [21]. Their 1-year study outcomes were also similar by using both IVR and IVA [22].
Garweg et al. [23] reported that both IVR and IVA showed the same functional and anatomical improvement in 24 months by using TE protocol. In this study, BCVA demonstrated an increase of 1.3 letters in IVR group and 0.6 letters in IVA group after 24 months when compared to the baseline. However, in this retrospective study, predominantly classical CNVs were treated with IVR but all others underwent IVA. In our study there were no difference according to CNV type between IVA and IVR groups. On the other hand, we demonstrated a BCVA increase of approximately five letters in both groups after 24 months. Our result could be explained by therapeutic tailoring. We also propose that following the patients in a single center, applying injections by the same method, conducting BCVA measurements by the same specialist, and checking the CMT by using same devices could provide more reliable results in terms of the real-life data.
A systemic review published by Ohji et al. [24] compared visual outcomes and treatment burden between IVR and IVA TE regimens in patients with nAMD at 2 years. In this study six randomized-controlled trials were analyzed. Both regimens were associated with comparable efficacy regarding the number of ETDRS letters gained vs. baseline after 2 years, however IVA TE was associated with six fewer injections than IVR TE [24]. But this study was based on randomized-controlled trials conducted under experimental conditions with tightly defined treatment algorithms, which might not fully reflect the posology used in real clinical practice.
In our study, both groups injection and visit numbers were similar (17.16 ± 3.98 in IVR group vs. 17 ± 4.13 in IVA group). Like other TE studies both groups’ visit numbers were not different [21-24]. After loading phase, both groups interval were prolonged 2 weeks equally. In our study both groups’ reactivation frequency were similar. Despite the fact that Aflibercept is usually administered at 2-month interval, with our results we can conclude both drugs efficiency is equal.
Regarding the weaknesses of this study; inclusion of relatively lower number of patients, presence of shorter follow-up period and choice of a retrospective analysis could be emphasized. However, the strengths of the present study include the following: all of the injections were implemented at a single center, BCVA was measured by the same specialist, CMT was measured by using the same device and strict follow-up criteria were performed.
In conclusion, in light of the real-life data obtained on the basis of 3-year IVR and IVA injections under a TE protocol, there were no significant differences between the IVR and IVA groups in terms of the BCVA, CMT, number of injections and number of patient visits. Although more intravitreal injections were performed in the 1st year, the need for intravitreal injections decreases in the 2nd and 3rd years. From the 3rd year onwards, intravitreal injection is sufficient in every 3 months for more than half of the patients.
Fig. 1
Total number of intravitreal injections over three years in intravitreal aflibercept (IVA) and intravitreal ranibizumab (IVR) groups.
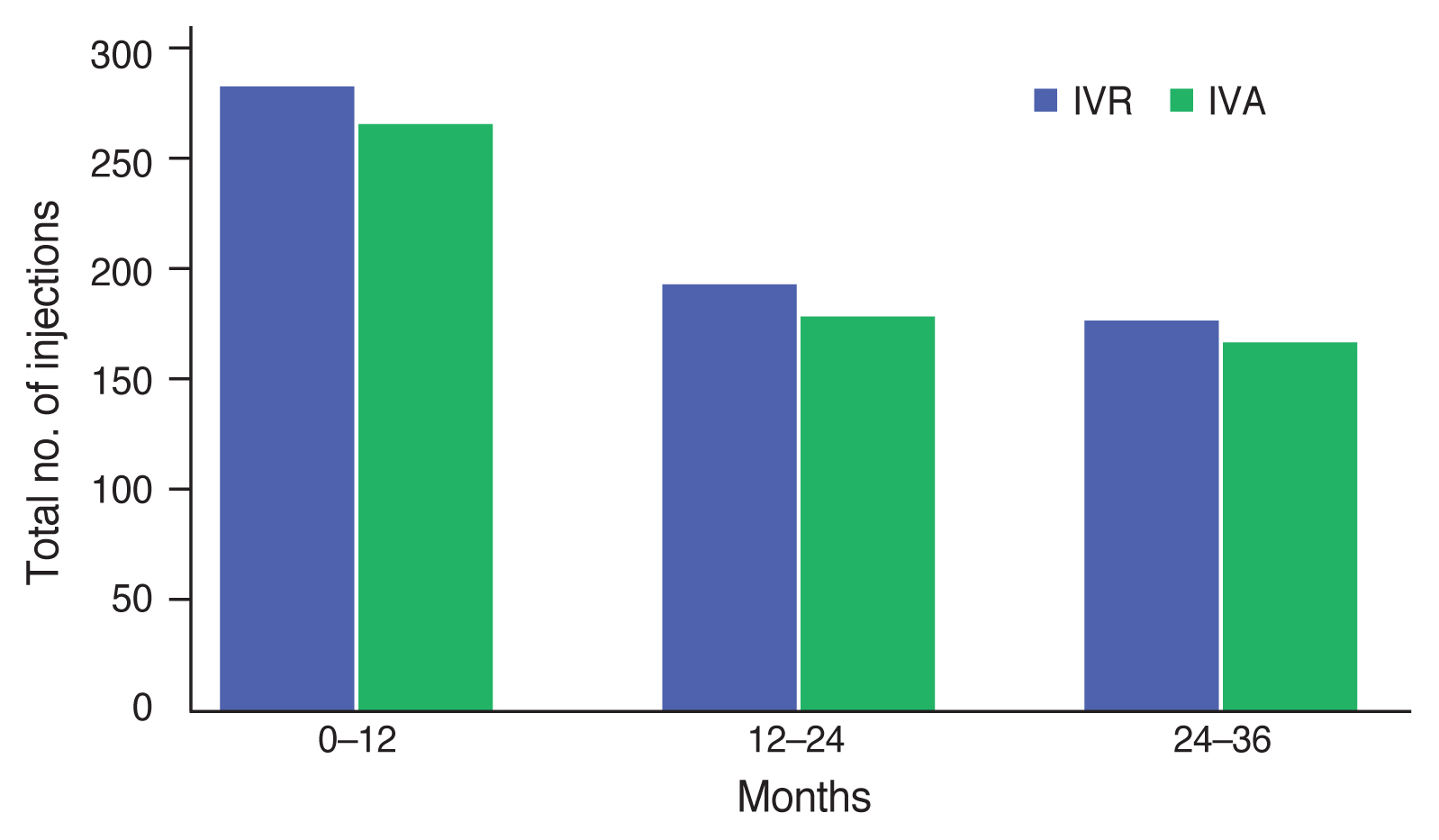
Fig. 2
Percentage of eyes and their average injection numbers during 1st, 2nd, and 3rd years in both groups. (A) Intravitreal ranibizumab and (B) intravitreal aflibercept.
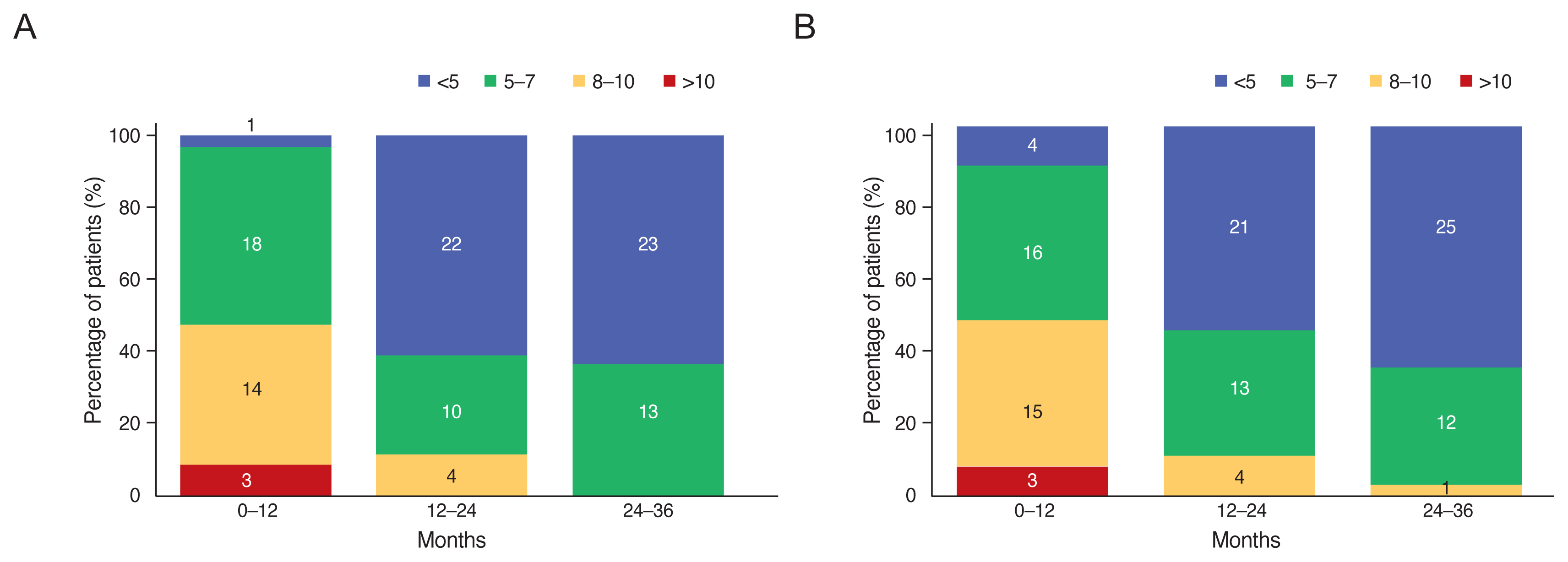
Fig. 3
Comparison of average (AVG) central macular thickness (CMT) and visual acuity (VA) changes during first, 2nd and 3rd years in both groups. IVA = intravitreal aflibercept.

Fig. 4
Comparison of average (AVG) changes of central macular thickness (CMT) and visual acuity (VA) during 1st, 2nd, and 3rd years in both groups. IVA = intravitreal aflibercept.
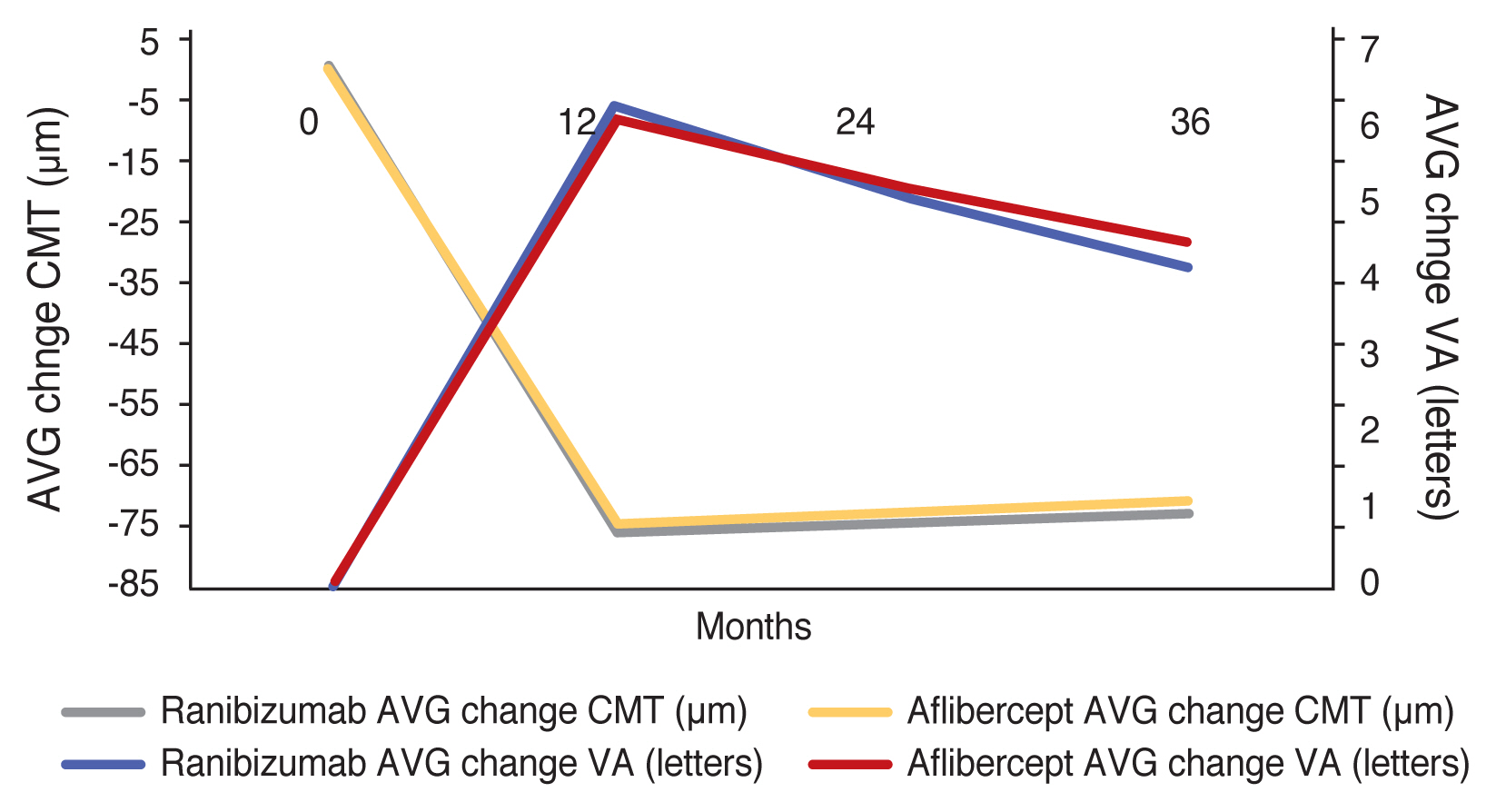
Table 1
Baseline characteristics for patients with neovascular age-related macular degeneration threated using a treat-and-extend regimen (n = 74 eyes)
Table 2
Visual and anatomical outcomes at 36 months in the intent-to-treat population (n = 74)
References
1. Li JQ, Welchowski T, Schmid M, et al. Prevalence and incidence of age-related macular degeneration in Europe: a systematic review and meta-analysis. Br J Ophthalmol 2020;104:1077-84.


2. Wong WL, Su X, Li X, et al. Global prevalence of age-related macular degeneration and disease burden projection for 2020 and 2040: a systematic review and meta-analysis. Lancet Glob Health 2014;2:e106-16..


3. Ozkaya A, Karabas L, Alagoz C, et al. Real-world outcomes of anti-VEGF treatment for neovascular age-related macular degeneration in Turkey: a multicenter retrospective study, Bosphorus Retina Study Group Report No: 1. Turk J Ophthalmol 2018;48:232-7.



4. Yamamoto-Rodriguez L, Zarbin MA, Casaroli-Marano RP. New frontiers and clinical implications in the pathophysiology of age-related macular degeneration. Med Clin (Barc) 2020;154:496-504.


5. Wolff B, Macioce V, Vasseur V, et al. Ten-year outcomes of anti-vascular endothelial growth factor treatment for neovascular age-related macular disease: a single-centre French study. Clin Exp Ophthalmol 2020;48:636-43.


7. Verner-Cole EA, Davis SJ, Lauer AK. Aflibercept for the treatment of neovascular age-related macular degeneration. Drugs Today (Barc) 2012;48:317-29.


8. Brown DM, Kaiser PK, Michels M, et al. Ranibizumab versus verteporfin for neovascular age-related macular degeneration. N Engl J Med 2006;355:1432-44.


9. Rosenfeld PJ, Brown DM, Heier JS, et al. Ranibizumab for neovascular age-related macular degeneration. N Engl J Med 2006;355:1419-31.


10. Heier JS, Brown DM, Chong V, et al. Intravitreal aflibercept (VEGF trap-eye) in wet age-related macular degeneration. Ophthalmology 2012;119:2537-48.


11. Schmidt-Erfurth U, Kaiser PK, Korobelnik JF, et al. Intravitreal aflibercept injection for neovascular age-related macular degeneration: ninety-six-week results of the VIEW studies. Ophthalmology 2014;121:193-201.


12. Distler O, Neidhart M, Gay RE, Gay S. The molecular control of angiogenesis. Int Rev Immunol 2002;21:33-49.


13. Lalwani GA, Rosenfeld PJ, Fung AE, et al. A variable-dosing regimen with intravitreal ranibizumab for neovascular age-related macular degeneration: year 2 of the PrONTO Study. Am J Ophthalmol 2009;148:43-58.


14. Karacorlu M, Hocaoglu M, Arf S, et al. Risk-based algorithm-guided treatment protocol for the management of neovascular age-related macular degeneration. Turk J Ophthalmol 2019;49:258-69.



15. Lanzetta P, Loewenstein A. Vision Academy Steering Committee. Fundamental principles of an anti-VEGF treatment regimen: optimal application of intravitreal anti-vascular endothelial growth factor therapy of macular diseases. Graefes Arch Clin Exp Ophthalmol 2017;255:1259-73.



16. Skelly A, Bezlyak V, Liew G, et al. Treat and extend treatment interval patterns with anti-VEGF therapy in nAMD patients. Vision (Basel). 2019. 3:p. 41.



17. Schmucker CM, Rucker G, Sommer H, et al. Treatment as required versus regular monthly treatment in the management of neovascular age-related macular degeneration: a systematic review and meta-analysis. PLoS One 2015;10:e0137866..



18. Augsburger M, Sarra GM, Imesch P. Treat and extend versus pro re nata regimens of ranibizumab and aflibercept in neovascular age-related macular degeneration: a comparative study. Graefes Arch Clin Exp Ophthalmol 2019;257:1889-95.


19. Spitzer MS, Ziemssen F, Bartz-Schmidt KU, et al. Treatment of age-related macular degeneration: focus on ranibizumab. Clin Ophthalmol 2008;2:1-14.



20. Berg K, Roald AB, Navaratnam J, Bragadottir R. An 8-year follow-up of anti-vascular endothelial growth factor treatment with a treat-and-extend modality for neovascular age-related macular degeneration. Acta Ophthalmol 2017;95:796-802.


21. Smit C, Wiertz-Arts K, van de Garde EM. Intravitreal aflibercept versus intravitreal ranibizumab in patients with age-related macular degeneration: a comparative effectiveness study. J Comp Eff Res 2018;7:561-7.


22. Gillies MC, Hunyor AP, Arnold JJ, et al. Effect of ranibizumab and aflibercept on best-corrected visual acuity in treat-and-extend for neovascular age-related macular degeneration: a randomized clinical trial. JAMA Ophthalmol 2019;137:372-9.



23. Garweg JG, Gerhardt C, Kodjikian L, Pfister IB. Real-life experience with aflibercept and ranibizumab in the treatment of newly diagnosed neovascular age-related macular degeneration over 24 months. J Ocul Pharmacol Ther 2017;33:567-72.


24. Ohji M, Lanzetta P, Korobelnik JF, et al. Efficacy and treatment burden of intravitreal aflibercept versus intravitreal ranibizumab treat-and-extend regimens at 2 years: network meta-analysis incorporating individual patient data meta-regression and matching-adjusted indirect comparison. Adv Ther 2020;37:2184-98.






 PDF Links
PDF Links PubReader
PubReader ePub Link
ePub Link Full text via DOI
Full text via DOI Full text via PMC
Full text via PMC Download Citation
Download Citation Print
Print




