 |
 |
| Korean J Ophthalmol > Volume 32(6); 2018 > Article |
Dear Editor,
Choroidal osteoma is an uncommon benign ossifying tumor involving the choroid and usually presents as an elevated choroidal lesion with round, ill-defined borders located in the juxtapapillary or macula region [1,2]. To date, the treatment for choroidal osteoma has not been established. Herein, we describe a case of a patient who underwent intravitreal ranibizumab injection for choroidal osteoma accompanied by proliferative diabetic retinopathy.
A 49-year-old male who was treated for proliferative diabetic retinopathy visited our clinic due to ocular pain in his right eye 4 days in duration. His past medical history included diabetes mellitus. His ophthalmic history showed high risk proliferative diabetic retinopathy in both eyes; the patient underwent photocoagulation at a local clinic. The initial best-corrected visual acuity was 0.04 in the right eye and 0.4 in the left eye. The initial intraocular pressure was 15 mmHg in the right eye and 14 mmHg in the left eye. Two years ago he was diagnosed with diabetic macular edema and intravitreal aflibercept injection was performed in our hospital. One month after the injection, subretinal fluid was completely absorbed. On slit-lamp examination, no abnormal findings were found except mild swelling in the right upper lid and diffuse hyperemia in the right conjunctiva. On fundus examination, a yellowish elevated lesion was observed in the macula of his right eye (Fig. 1A). Fluorescein angiography showed no leakage and mild staining at the perifoveal area at late phase (Fig. 1B). Our initial diagnosis was suspicious choroidal mass with diabetic macular edema in the right eye and upper lid preseptal cellulitis in the right eye. Therefore, ultrasonography and orbital computed tomography with enhancement were performed. Highly reflective echo and posterior acoustic shadowing were observed in his right eye (Fig. 1C). Orbital computed tomography showed mild infiltration at the anterior ocular wall, asymmetrical swelling of lacrimal gland, and small calcification at posterior ocular wall (Fig. 1D, 1E). Optical coherence tomography (Spectralis, Heidelberg Engineering, Heidelberg, Germany) also showed an elevated mass lesion and subretinal fluid with small choroidal neovascularization (CNV) in the right eye (Fig. 1F). The patient was prescribed oral antibiotics, levofloxacin eyedrops, and fluorometholone eyedrops.
After 2 days, upper lid swelling significantly decreased and conjunctival injection was improved. However, optical coherence tomography showed persistent subretinal fluid. The patient was finally diagnosed with choroidal osteoma with subretinal fluid. Intravitreal ranibizumab (Novartis, East Hanover, NJ, USA) injection was performed (0.05 mL) and 1 month after the injection, subretinal fluid was completely absorbed and visual acuity recovered from 0.04 to 0.2 (Fig. 1G).
Choroidal osteoma often occurs as a unilateral condition in young females and supposedly associated with congenital causes, inflammatory conditions, and endocrine disorders; however, the origin is unclear [1]. Fluorescein angiography of choroidal osteoma shows punctate hyperfluorescence at early phase and diffuse staining at late phase. In addition, ultrasonography shows a strong reflection wave on the inner surface of the tumor and computed tomography shows radiopacity in accordance with bone density.
The treatment for choroidal osteoma has not yet been established and the patient is usually under observation if there is no active lesion. However, various treatments have been attempted if CNV or subretinal fluid are present. Previously, photocoagulation was typically used for extrafoveal CNV, and subfoveal CNV was treated with transpupillary thermotherapy or photodynamic therapy. However, there are many drawbacks such as limited final visual acuity. Recently, several cases were treated with anti-vascular endothelial growth factor drugs used in age-related macular degeneration or diabetic macular edema such as bevacizumab or ranibizumab [3,4]. Najafabadi et al. [3] reported improvement in a patient treated with intravitreal bevacizumab for choroidal osteoma without CNV.
In our patient, subretinal fluid with small CNV was observed in the choroidal osteoma accompanied by proliferative diabetic retinopathy. Improvement of subretinal fluid and visual acuity were observed 1 month after intravitreal ranibizumab injection. Therefore, we suggest that intravitreal ranibizumab injection may be a useful treatment for the subretinal fluid associated with choroidal osteoma.
Acknowledgements
This study was financially supported by Korean Association of Retinal Degeneration.
Notes
Conflict of Interest: No potential conflict of interest relevant to this article was reported.
REFERENCES
1. Alameddine RM, Mansour AM, Kahtani E. Review of choroidal osteomas. Middle East Afr J Ophthalmol 2014;21:244-250.



2. Shields CL, Sun H, Demirci H, Shields JA. Factors predictive of tumor growth, tumor decalcification, choroidal neovascularization, and visual outcome in 74 eyes with choroidal osteoma. Arch Ophthalmol 2005;123:1658-1666.


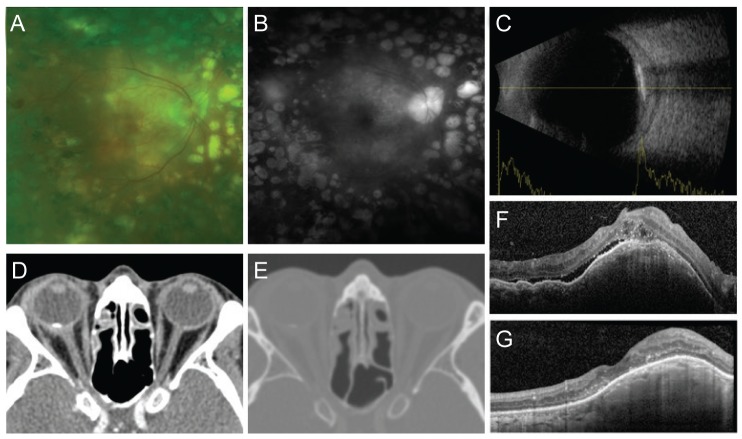
Fig. 1
(A) At fundus photography, yellowish elevated lesion with irregular margin was noted. (B) On fluorescein angiography, mild staining was observed for perifoveal area at late phase. (C) Highly reflective echo and posterior acoustic shadowing were observed in the ultrasonography. (D) Computed tomography showed mild infiltration at anterior ocular wall, asymmetrical swelling of lacrimal gland, and small calcif ication at posterior wall. (E) Computed tomography scan with bone density. (F) At initial examination, optical coherence tomography showed subretinal fluid with small choroidal neovascularization. (G) A month after intravitreal ranibizumab injection, subretinal fluid was completely absorbed.
- TOOLS
-
METRICS

-
- 1 Crossref
- 0 Scopus
- 2,168 View
- 14 Download
- Related articles
-
Orbital Venous Malformation Accompanied by Arteriovenous Fistula2020 August;34(4)
Vitrectomy for severe proliferative diabetic retinopathy.1994 December;8(2)



 PDF Links
PDF Links PubReader
PubReader Full text via DOI
Full text via DOI Full text via PMC
Full text via PMC Download Citation
Download Citation Print
Print



