 |
 |
| Korean J Ophthalmol > Volume 28(1); 2014 > Article |
Abstract
Purpose
To evaluate the effectiveness of silicone oil tamponade in patients with chronic serous retinal detachment (SRD) persisting for three months after the resolution of ocular inflammation.
Methods
A total of 17 eyes of 17 patients diagnosed with chronic SRD persisting for three months after the resolution of ocular inflammation and with high risk of phthisis bulbi by secondary ocular hypotony and macular detachment by subretinal fibrous membrane formation were subjected to surgical intervention. Subjects underwent silicone oil tamponade after surgical drainage of subretinal fluid. Retrospective analyses on anatomical and functional success rates were then performed.
Results
Anatomical success with retinal reattachment was observed in ten of the 17 eyes (58.82%), while functional success measured as difference in the best-corrected visual acuity before and after the surgery were logarithm of the minimum angle of resolution (logMAR) 1.95 ± 0.66 and logMAR 1.51 ± 0.66, respectively (p < 0.05).
Excess choroidal fluid leakage, as occurs with inflammatory or systemic diseases such as hematologic disorders or tumors, can result in serous retinal detachment (SRD). The accumulation of subretinal fluid leads to SRD without retinal tears or vitreoretinal traction.
Causes of SRD include Vogt-Koyanagi-Harada syndrome [1], choroidal melanoma [2], Coats' disease [3], uveal effusion syndrome [4], exudative age-related macular degeneration [5], inflammatory bowel disease [6], sarcoidosis [7], and infections [8]. SRD is also seen with systemic diseases such as pregnancy-induced hypertension, malignant hypertension, connective tissue disorders, vascular disorders, and disseminated intravascular coagulation [9]. The primary treatment for SRD is to target the disease process itself; infections are controlled with antibiotics and inflammation with anti-inflammatory therapies. Most of the time, SRD resolves with medication. However, SRD occasionally persists for several months or years, despite the resolution of inflammation. When this occurs, it can induce the formation of a subretinal fibrous membrane, and the retina may fail to permanently reattach. Chronic SRD can also lead to ocular hypotony and phthisis bulbi.
We retrospectively reviewed the medical records of patients whose SRD was treated with surgical intervention after the resolution of ocular inflammation. The purpose of this study was to evaluate the anatomical and functional success rates of surgical drainage and silicone oil tamponade for SRD.
The study population included patients of Wonkwang University Hospital who demonstrated SRD due to inflammatory conditions despite preoperative medical treatment during the period of March 2001 to December 2012. Seventeen patients (17 eyes) underwent 23-gauge transconjunctival sutureless vitrectomy, surgical subretinal fluid removal, and silicone oil tamponade to address persistent subretinal fluid. The medical records of these patients were reviewed retrospectively. All patients were diagnosed, treated, and operated on by a single surgeon.
Patients initially underwent medical treatments consisting of oral steroids, posterior sub-Tenon triamcinolone injection (40 mg/mL), or intravitreal triamcinolone acetonide injection (4 mg/0.1 mL) either individually or in combination. Subjects who were 20 years or older were prescribed with oral steroids 40 mg for the first two weeks, and then the dose was reduced by half to 20 mg for the next two weeks. The dose was reduced by half again for a final dose of 10 mg for one month. Patients who were younger than 20 years were given 20 mg for the first two weeks. The tapering protocol was the same for both groups. Treatment options were chosen according to the patient's condition and treatment trends at that time. The patients who had persisting SRD for more than three months despite preoperative medical treatment and with high risk of phthisis bulbi from ocular hypotony and macular detachment from subretinal fibrous membrane formation were subjected to the surgical intervention outlined below. Patients were briefed in detail about the procedure, and written consent was obtained.
Retrobulbar anesthesia was performed with a 1 : 1 mixture of 2% lidocaine and 0.75% bupivacaine. Sutureless total vitrectomy was performed using both a 23-gauge cannula system and a Millennium microsurgical system (Bausch and Lomb, Rochester, NY, USA). Patients with subretinal fibrous membrane underwent removal of this structure. The rest of the patients underwent subretinal fluid removal and air-fluid exchange and achieved reattachment of the retina. Air was exchanged with silicone oil (5,000 centistokes). Drainage retinotomy was performed around the optic disc.
We removed silicone oil only when stable reattachment of the retina on the fundus exam and no fluorescence leakage on fluorescein angiography (FAG) were observed. We also removed the oil when unmanageable complications associated with injected oil occurred.
Intraocular pressure was measured using a Goldman applanation tonometer or non-contact tonometer at the first visit, preoperatively, postoperatively, and at the final follow-up, the last of which occurred at least more than six months after silicone oil removal. The Snellen eye chart was used to assess best-corrected visual acuity, which was then converted to logarithm of the minimum angle of resolution (logMAR) value. We evaluated postoperative complications using slit lamp biomicroscopy and dilated fundus examination. We used FAG to assess subretinal fluid leakage.
The analysis of surgical outcomes was divided into anatomical and functional success. Anatomical success was defined as total reattachment of the retina during the follow-up period. Functional success was defined as visual improvement. The difference between first-visit and preoperative visual acuity (VA) and that between preoperative and final VA were assessed in logMAR.
All analyses were performed with SPSS ver. 12.0 (SPSS Inc., Chicago, IL, USA). Wilcoxon's signed-rank test was employed to compare changes in VA. Two-tailed p-values less than 0.05 were considered to have statistical significance.
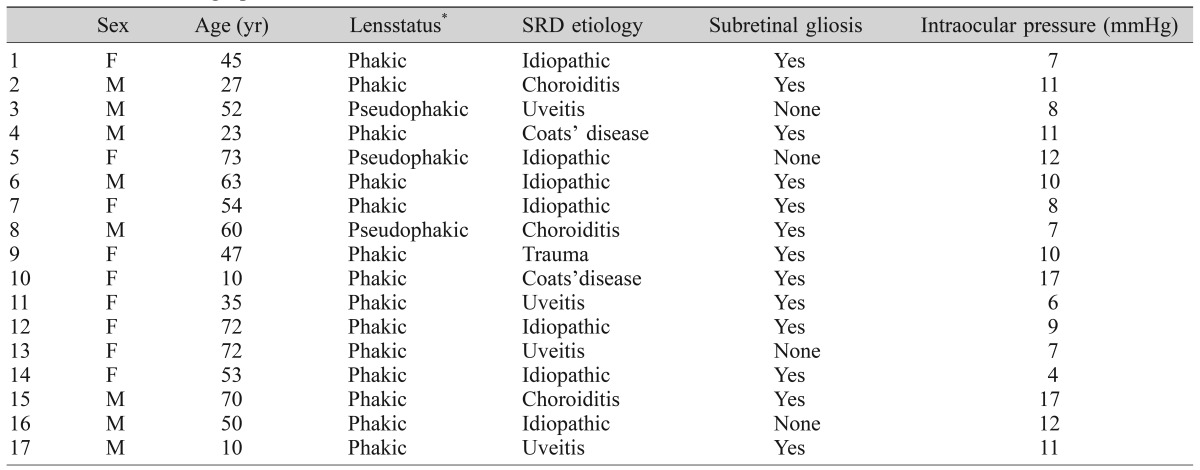
The demographics of the study group are listed in Table 1. The study population consisted of eight males and nine females. Their mean age was 48.00 ± 20.68 years. Among 17 eyes, 14 eyes were phakic and three eyes were pseudophakic. The causes of SRD were idiopathic uveitis (4 eyes), idiopathic choroiditis (3 eyes), Coats' disease (2 eyes), trauma (1 eye), and unknown (7 eyes).
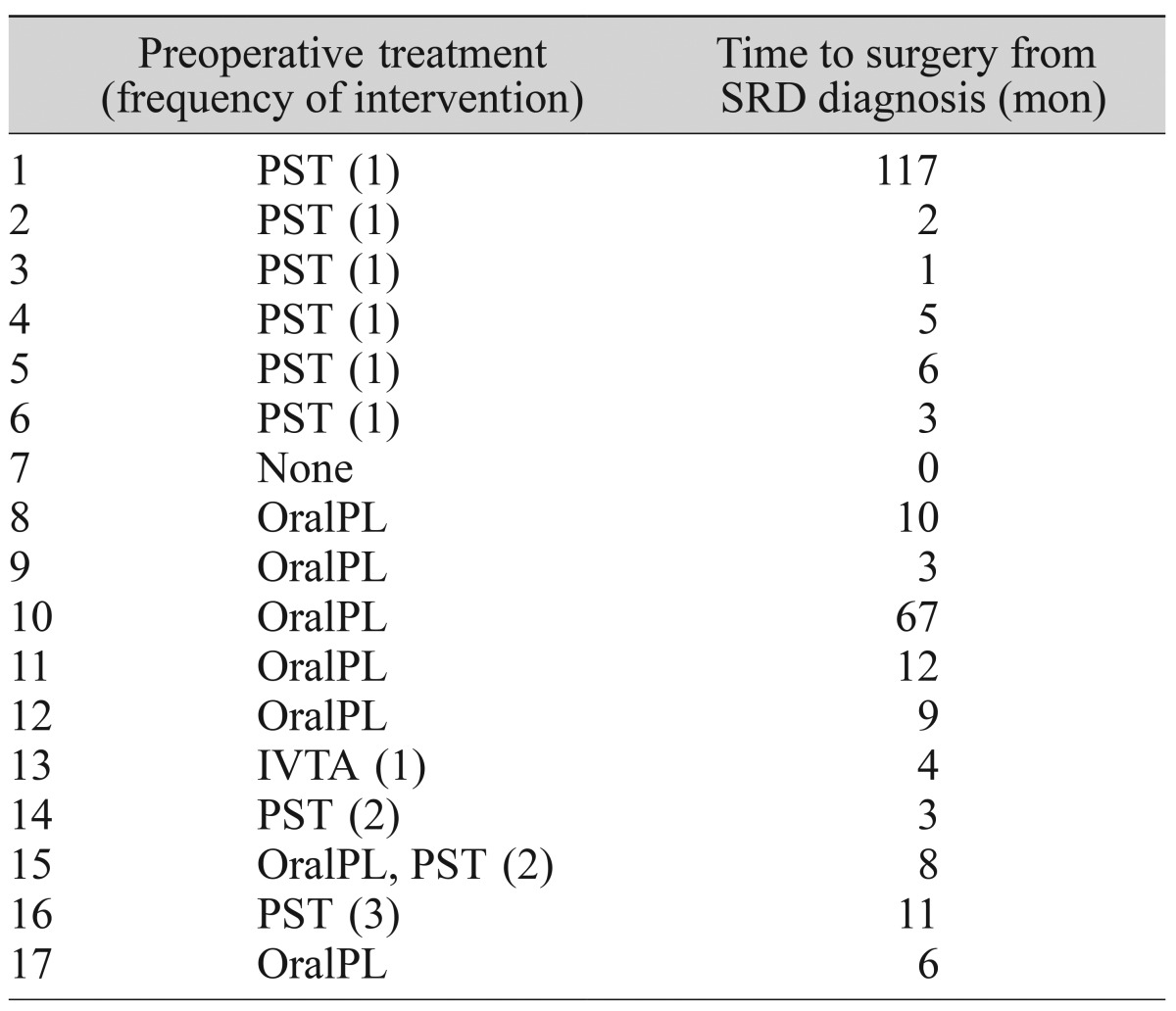
For preoperative treatment (Table 2), eight eyes of the study population were treated with posterior sub-Tenon triamcinolone injection, six eyes with oral steroids, and one eye with a combination of the aforementioned two methods. One eye underwent intravitreal triamcinolone acetonide injection. One eye was immediately subjected to surgical intervention without any prior treatment as long-lasting SRD induced a subretinal proliferative fibrous membrane and macular detachment. The mean follow-up time from medical treatment to operation for the remaining 16 eyes was 9.28 ± 15.40 months (Table 2).
The mean time for silicone oil tamponade was 13 ± 11.71 months. The patients were followed for a mean time of 28.24 ± 27.31 months after silicone oil removal (Table 3).
At the final follow-up, the anatomical success rate was 82.35% (14 eyes). The actual anatomical success rate, however, was 58.82% as three eyes did not require silicone oil removal, and one eye underwent re-tamponade due to retinal re-detachment following oil removal. Two eyes showed persistent inferior-retinal detachment after oil injection; one eye was managed by observation as the detachment did not progress following oil removal (Table 4).
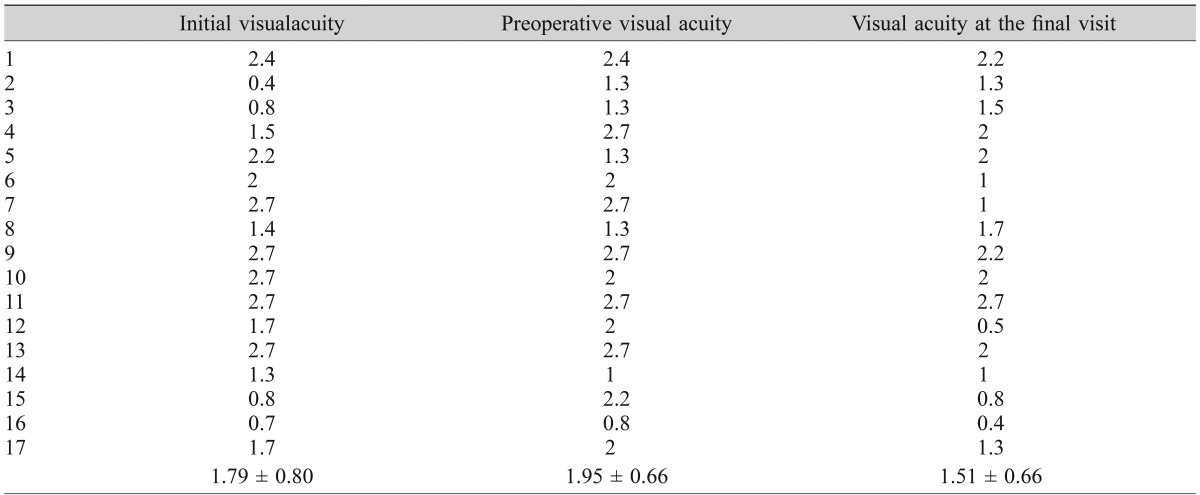
While mean VA at the time of diagnosis of SRD was logMAR 1.79 ± 0.80, preoperative VA after medical treatment decreased to logMAR 1.95 ± 0.66, but this difference was not statistically significant (p = 0.285). Mean VA at the final follow-up improved to logMAR 1.51 ± 0.66, showing a significant difference from preoperative VA (p = 0.021) (Table 5).
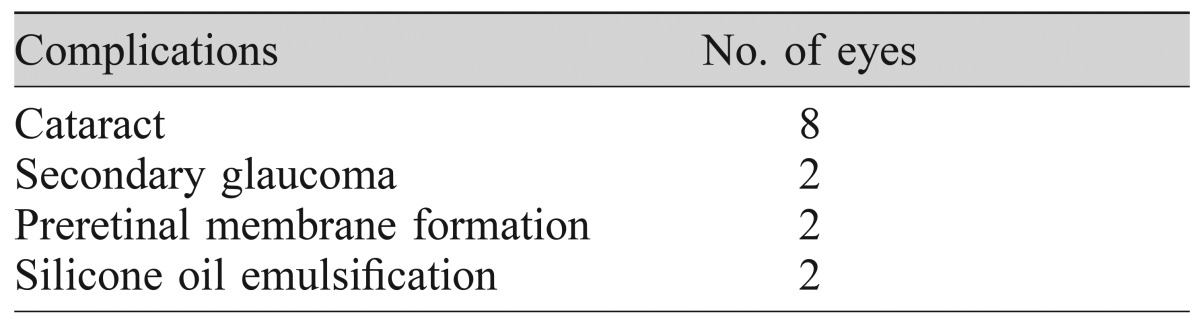
Several complications occurred during the study. Cataract developed in eight eyes, accounting for 57.14% of phakic eyes after silicone oil injection. Therefore, we performed cataract surgery at the time of the silicone oil removal. In addition, two eyes with secondary glaucoma, two eyes with preretinal membrane, and two eyes with emulsified silicone oil were noted (Table 6).
As mentioned earlier, there are a variety of conditions that can induce SRD. The primary treatment for this disorder is improving the underlying disease itself so that the abnormal fluid leakage can be stopped. Specifically, SRD associated with uveitis is treated using oral anti-inflammatory agents, sub-Tenon triamcinolone injection, and intravitreal triamcinolone acetonide injection. Retinal reattachment can be obtained through the resorption of physiologic subretinal fluid.
There are circumstances where anti-inflammatory agents resolve inflammation but fail to result in retinal reattachment due to persistent subretinal fluid. This fluid may play a role in prohibiting resorption by creating high oncotic pressure that can lead to fluid leakage. In addition, secondary ocular hypotony may lead to phthisis bulbi. In cases involving a subretinal proliferative fibrous membrane, permanent reattachment of the retina can rarely be achieved. Thus, we eliminated pathologic high oncotic pressure created by subretinal fluid through surgical drainage and subsequent silicone oil tamponade. The surgical intervention was considered to offer a normal trans-retinal pressure gradient, reduced damage of retinal pigmentary epithelium and photoreceptors, and a tamponade effect from the silicone oil. These characteristics may induce visual improvement through ocular stabilization and retinal reattachment.
In 2008, Galor et al. [10] evaluated the outcomes of surgical management in chronic SRD associated with uveitis in five eyes. They reported that retinal reattachment was achieved in all patients within a median 55-month follow-up period, and four of five patients experienced improvement in VA. They suggested a treatment algorithm that includes surgical intervention for SRD associated with ocular inflammation that persists for three months after resolution of the primary disorder. In the present study, ten of 17 eyes (58.82%) showed stable reattachment of the retina and statistically significant improvement of VA (p = 0.021) after surgical drainage.
Silicone oil tamponade has been used as a vitreous substitute in vitreoretinal surgery. The indications are complex retinal detachment or proliferative diabetic retinopathy accompanied by tractional retinal detachment. It also can be used when a patient has difficulty maintaining fixed same position and to prevent pthisis bulbi. Silicone oil tamponade is also indicated for the prevention of fibrous membrane proliferation due to complex operation or damage and to preserve the eyeball in cases of severe trauma [11]. However, this approach can have complications that include migration of oil into the anterior chamber, cataract, cornea dysfunction, elevated intraocular pressure, and proliferation of the epiretinal membrane. Another shortcoming is the requirement of a second operation to remove the oil [12].
In our study, eight of 14 phakic eyes (57.14%) developed cataract after silicone oil tamponade. We consequently performed cataract surgery at the time of silicone oil removal. In the case of two eyes demonstrating a proliferative membrane in the macula, we simultaneously removed both the silicone oil and membrane. Another two eyes with glaucoma caused by elevated intraocular pressure were treated with eye-drops.
This study had several limitations. Uveitis has a high tendency to recur, so patients require follow-up. Moreover, it is possible that the SRD would have eventually spontaneously resolved with time. Therefore, further studies are needed regarding the appropriate timing of surgical intervention. Other limitations include the small sample size and absence of a control group. Although further study with a larger group in a prospective fashion is warranted, this study's approach provides a certain value by demonstrating resolution of chronic SRD using surgical methods.
In conclusion, in patients with SRD persisting after medical treatment or with SRD at risk of developing pthisis bulbi or macular detachment, surgical drainage of subretinal fluid with silicone oil tamponade can achieve anatomical and functional success.
REFERENCES
1. Kiyomoto C, Imaizumi M, Kimoto K, et al. Vogt-Koyanagi-Harada disease in elderly Japanese patients. Int Ophthalmol 2007;27:149-153.


2. Folk JC, Weingeist TA, Coonan P, et al. The treatment of serous macular detachment secondary to choroidal melanomas and nevi. Ophthalmology 1989;96:547-551.


3. Otani T, Yamaguchi Y, Kishi S. Serous macular detachment secondary to distant retinal vascular disorders. Retina 2004;24:758-762.


4. Uyama M, Takahashi K, Kozaki J, et al. Uveal effusion syndrome: clinical features, surgical treatment, histologic examination of the sclera, and pathophysiology. Ophthalmology 2000;107:441-449.


5. Carvounis PE, Kopel AC, Benz MS. Retinal pigment epithelium tears following ranibizumab for exudative age-related macular degeneration. Am J Ophthalmol 2007;143:504-505.


6. Ernst BB, Lowder CY, Meisler DM, Gutman FA. Posterior segment manifestations of inflammatory bowel disease. Ophthalmology 1991;98:1272-1280.


7. Watts PO, Mantry S, Austin M. Serous retinal detachment at the macula in sarcoidosis. Am J Ophthalmol 2000;129:262-264.


8. Gupta A, Gupta V, Arora S, et al. PCR-positive tubercular retinal vasculitis: clinical characteristics and management. Retina 2001;21:435-444.


9. Karaguzel H, Guven S, Karalezli A, Erdol H. Bilateral serous retinal detachment in a woman with HELLP syndrome HELLP syndrome and retinal detachment. J Obstet Gynaecol 2009;29:246-248.


10. Galor A, Lowder CY, Kaiser PK, et al. Surgical drainage of chronic serous retinal detachment associated with uveitis. Retina 2008;28:282-288.


- TOOLS
-
METRICS

- Related articles
-
Neovascular Glaucoma Associated with Chronic Rhegmatogenous Retinal Detachment2023 June;37(3)






 PDF Links
PDF Links PubReader
PubReader Full text via DOI
Full text via DOI Full text via PMC
Full text via PMC Download Citation
Download Citation Print
Print



