 |
 |
| Korean J Ophthalmol > Volume 28(2); 2014 > Article |
Abstract
Purpose
Single umbilical artery (SUA) is the most common malformation of the umbilical cord. However, there have been no studies on the ocular findings in SUA, except for one case report. This study aimed to investigate the ocular findings in children with SUA.
Methods
Fourteen children (eight boys and six girls) with SUA were evaluated retrospectively. All children underwent a complete ophthalmologic examination.
Results
The prevalence of abnormal ocular findings in children was up to 42.9%. Refractive errors are detected in four eyes (14.3%): myopia Ōēź-1.50 diopters (D) in one eye (3.6%) and hyperopia Ōēź+2.00 D in three eyes (10.7%). Epiblepharon was found in three children (21.4%), and strabismus was detected in one child (7.1%).
Umbilical cord vessels are composed of two arteries and one vein. Single umbilical artery (SUA) is the result of either aplasia or atresia of one of the two umbilical arteries [1]. SUA is the most common malformation of the umbilical cord, found in 0.2% to 1.0% of pregnancies [2]. SUA has been of interest because of its association with congenital anomalies, perinatal death, premature delivery and growth retardation. Detected congenital anomalies involve the urogenital, gastrointestinal, cardiovascular, respiratory, and central nervous systems [3]. However, there have been no studies on ocular findings in SUA, except for one case report on the occurrence of microphthalmia and congenital glaucoma [4]. The purpose of our study was to characterize ocular features in children with SUA and to provide evidence of the efficacy of ophthalmic screening in such children.
This is a retrospective case series study of 14 children (eight boys and six girls). Between January 2004 and March 2008, we performed a retrospective review of the medical records of 14 children with SUA at the Seoul National University Bundang Hospital. SUA was diagnosed using prenatal ultrasonography and confirmed by a naked-eye examination of the umbilical cord after delivery. All aspects of the research protocol were in compliance with the Declarations of Helsinki. The age at examination was 28.7 ┬▒ 16.5 months (range, 12 to 60 months). The gestational age was 35.5 ┬▒ 3.3 weeks (range, 32 to 40 weeks) and the number of children who were born at preterm and full-term were nine and five, respectively.
Complete ophthalmic evaluations were performed in all children with SUA, including measurement of visual acuity, either the Krimsky test or the prism and alternate-cover testing with accommodative fixation targets at 1/3 and 6 m, a slit-lamp biomicroscopic examination, cycloplegic refractions, and fundus examination.
Visual acuity was measured using a letter chart if possible. In children whose visual acuity could not be measured with a letter chart, the CSM (central, steady, maintained) method was taken into account according to the fixation pattern. Refractive errors were determined using cycloplegic refraction with cyclopentolate hydrochloride 1% and analyzed as spherical equivalent values. Myopia was defined as the spherical equivalent refraction of at least -1.50 diopters (D), hyperopia as the spherical equivalent refraction of at least +2.00 D. Values obtained for all parameters are expressed as mean ┬▒ standard deviation.
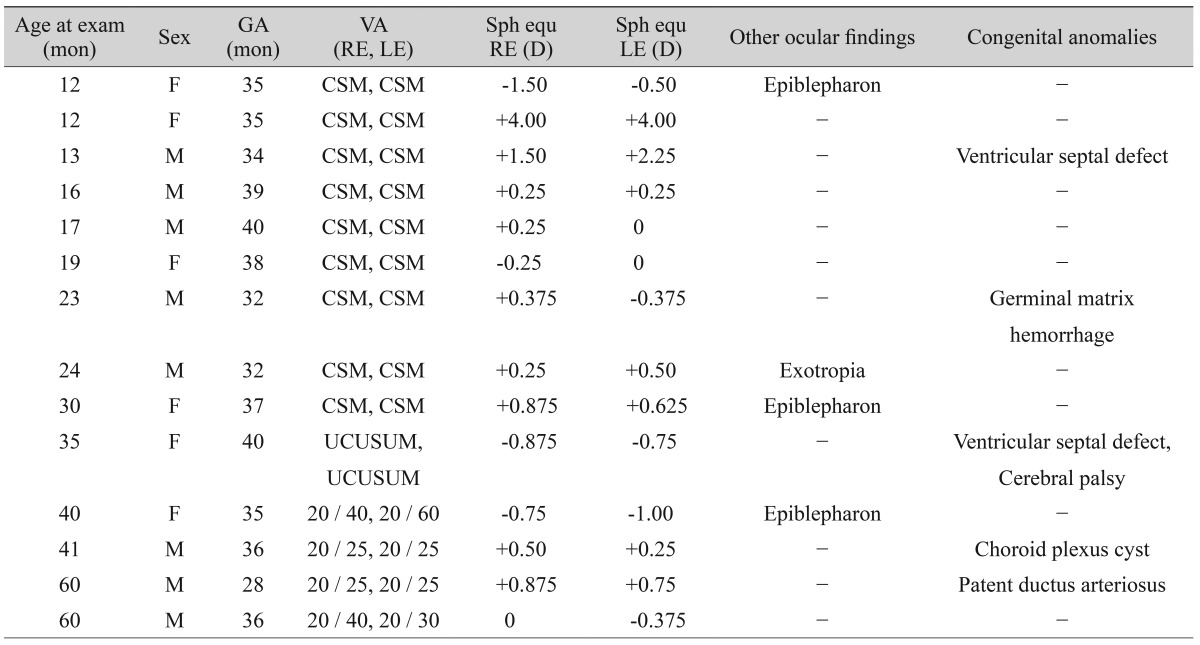
The prevalence of abnormal ocular findings in children was 42.9%. The most common ocular findings were refractive errors, epiblepharon, and strabismus. Congenital anomalies involving the cardiovascular and central nervous systems were detected in five children (35.7%). Chromosomal abnormalities were not detected in any child. There was no statistically significant relationship between congenital anomalies and abnormal ocular findings (p = 0.715, Fisher's exact test) (Table 1).
Mean spherical equivalent was +0.39 ┬▒ 1.27 D. Refractive errors were detected in four eyes (14.3%): myopia Ōēź-1.50 D in one eye (3.6%) and hyperopia Ōēź+2.00 D in three eyes (10.7%) (Table 2). Visual acuity could only be measured with the CSM method in 10 children. Of these, nine children had central, steady and maintained vision bilaterally and one child with cerebral palsy showed uncentral, unsteady and unmaintained vision bilaterally. The remaining four children were able to cooperate with vision testing and seven of eight eyes (87.5%) had a visual acuity of 20/40 or better (Table 1).
Epiblepharon involving the lower eyelid was found in three children (21.4%). In one child, there was inferior punctuate corneal epithelial erosion. Exotropia of 15 prism diopters at distance was detected in one child (7.1%) (Table 1). Slit-lamp biomicroscopic examination and fundus examination showed normal findings in all eyes. None of the children exhibited microphthalmia or congenital glaucoma, which has been reported in a previous study [4].
The primary objective of this study was to identify the ocular features of children with SUA. To the best of our knowledge, there has not yet been any case series study done investigating ocular features in children with SUA, and there has only been one case report about a child with SUA and microphthalmia [4]. In order to explore the ocular characteristics of children with SUA, we carried out a retrospective study and found a high prevalence of ocular abnormalities in this group, implying a relationship between SUA and ocular abnormalities.
In this study, we found that the most common ocular abnormalities associated with SUA were refractive errors, epiblepharon, and strabismus. In children with SUA, myopia Ōēź-1.50 D or hyperopia Ōēź+2.00 D were detected in four eyes (14.3%), although the prevalence of refractive errors was slightly lower than in Korean children of age 3 (21.0%) [5]. Epiblepharon (three subjects) and strabismus (one subject) also occurred in this group of children, with the prevalence of epiblepharon (21.4%) slightly higher in this group than the 16.5% prevalence of epiblepharon in normal Japanese children aged 3 to 4 years [6]. The prevalence of strabismus (7.1%) was similar to that (6.5%) of Korean children aged 3 [5].
When evaluating refractive errors, epiblepharon, and strabismus individually, there was no significant difference in the prevalence of each disease among children with SUA compared to the normal population. However, a key finding in this study was that when examining ocular abnormalities as a whole, the high prevalence of such abnormalities in children with SUA (up to 42.9% as shown in our study) demonstrates the necessity of evaluating all children diagnosed with SUA.
There are some potential weaknesses of our study. First, the sample size was relatively small in order to show statistically significant results. Second, the retrospective design of this study detracts from the solidity of the research findings. Third, although there was no statistically significant association between abnormal ocular findings and congenital anomalies, the congenital malformations could be a predisposing factor to ocular abnormalities in SUA. In order to overcome these weaknesses, it is necessary to perform a large prospective multicenter study of the ocular findings of children with SUA.
Even with these limitations, this is the first case series study ever to be done investigating ocular abnormalities in children with SUA. This study showed that the prevalence of abnormal ocular findings in patients with SUA was quite high (42.9%), including refractive errors (14.3%), epiblepharon (21.4%), and strabismus (7.1%). Therefore, a comprehensive ocular examination should be necessary in all children with SUA. Also, larger prospective clinical studies are warranted to determine the relationship between SUA and ocular abnormalities.
REFERENCES
2. Bryan EM, Kohler HG. The missing umbilical artery. I. Prospective study based on a maternity unit. Arch Dis Child 1974;49:844-852.



3. Byrne J, Blanc WA. Malformations and chromosome anomalies in spontaneously aborted fetuses with single umbilical artery. Am J Obstet Gynecol 1985;151:340-342.


4. Scalercio F, Ferraro M, Mastrantonio P, Scalercio A. Single umbilical artery (SUA) and congenital eye abnormalities: 2 case reports. Minerva Pediatr 1998;50:141-144.

5. Choi KS, Han YK, Park SH, Shin HH. Ophthalmic examinations in premature infants at 3 years of age. J Korean Ophthalmol Soc 2000;41:965-972.
- TOOLS




 PDF Links
PDF Links PubReader
PubReader Full text via DOI
Full text via DOI Full text via PMC
Full text via PMC Download Citation
Download Citation Print
Print




